Keratoconus Explained: Early Signs, Diagnosis, and Treatment Options
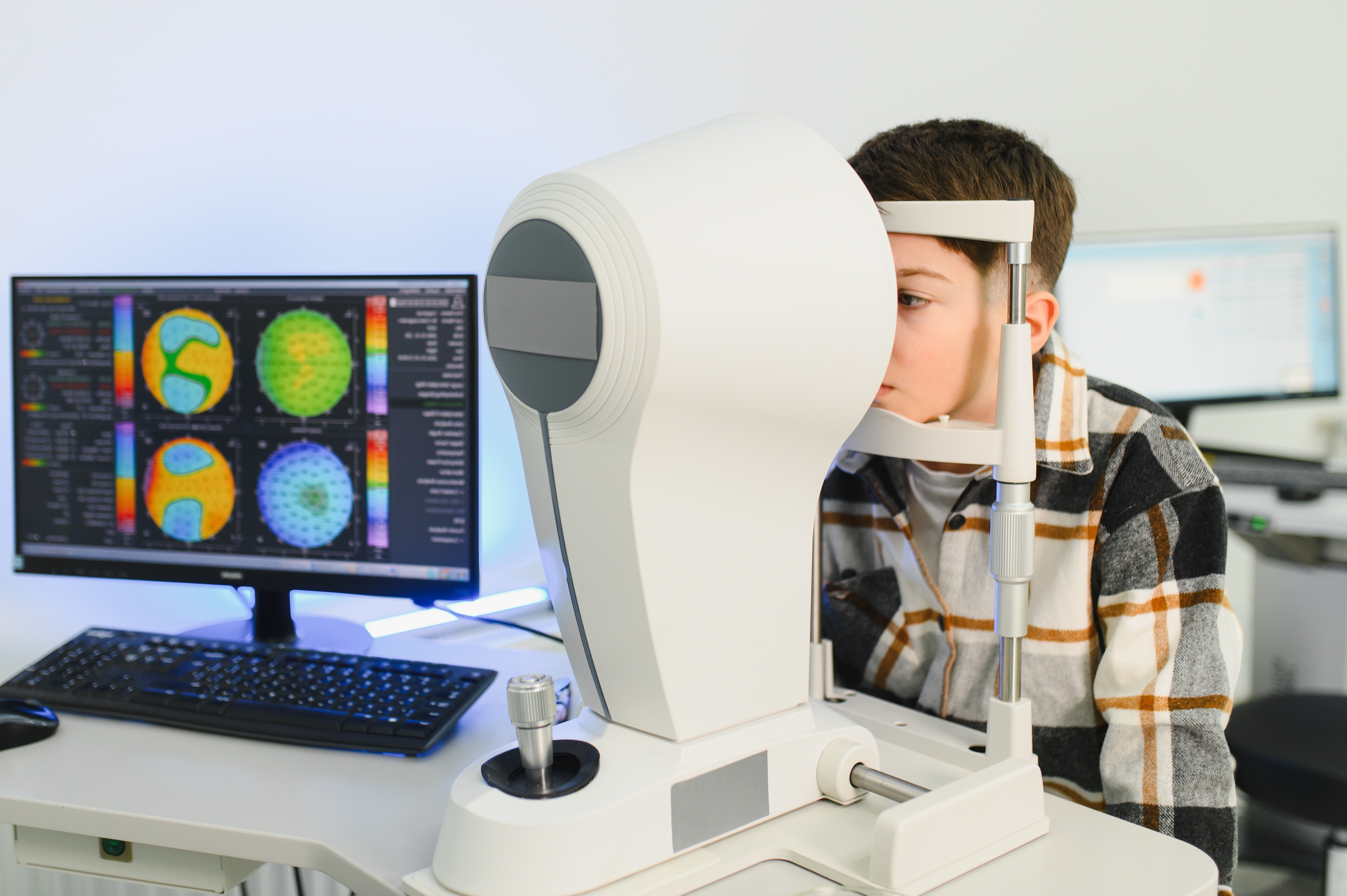
Clear, sharp vision depends on the precise shape of your cornea, the clear, dome-like front surface of your eye. When this structure changes, your entire world can look different. Keratoconus is a progressive eye condition where the normally round cornea thins and begins to bulge outward into a cone shape. This change alters how light enters the eye, leading to distorted and blurred vision that cannot always be corrected with standard glasses.
Understanding keratoconus is the first step toward managing it effectively. With today’s advanced diagnostic tools and specialized treatments, it is possible to slow the progression of the condition and restore clear, comfortable vision. This information will walk you through what keratoconus is, its early warning signs, how it is diagnosed, and the modern treatment options available to protect your sight.
What Is Keratoconus?
Keratoconus is a non-inflammatory eye condition that affects the structure of the cornea. In a healthy eye, the cornea is smooth and spherical, acting like a camera lens to focus light onto the retina at the back of the eye. Tiny protein fibers called collagen help hold the cornea in its round shape, keeping it strong and stable.
In an eye with keratoconus, these collagen fibers weaken. This structural weakness causes the cornea to lose its shape. The constant pressure from within the eye pushes the thinning cornea outward, causing it to bulge into an irregular, cone-like shape. This process typically begins during the teenage years or early twenties and can progress at different rates for each person.
How the Cornea Changes in Keratoconus
The primary change in keratoconus is the progressive thinning and steepening of the cornea. Instead of being a uniform dome, the cornea develops an irregular, asymmetric bulge. This bulge is often located in the lower half of the cornea.
As the cornea becomes more cone-shaped, its surface is no longer smooth. This irregularity disrupts the clean path of light entering the eye. The light rays bend and scatter in unpredictable ways, failing to converge at a single focal point on the retina. The result is a distorted and blurry image, similar to looking through a warped window. This structural change is what sets keratoconus apart from common refractive errors like myopia (short-sightedness) or astigmatism, although it often causes both.
Why Keratoconus Affects Vision
Your ability to see clearly is entirely dependent on light being focused precisely onto your retina. The cornea is responsible for about two-thirds of the eye's total focusing power. When keratoconus warps the cornea, it severely disrupts this focusing process.
The irregular corneal surface creates multiple focal points instead of just one. This means that light rays entering your eye are scattered rather than focused, leading to significant visual distortions. Standard glasses and soft contact lenses are designed to correct uniform refractive errors on a regularly shaped cornea. They are often unable to compensate for the complex, irregular astigmatism caused by the cone-shaped bulge of keratoconus, which is why vision may remain blurry even with a new prescription.
Early Signs and Symptoms of Keratoconus
Keratoconus often develops slowly, and its initial symptoms can be subtle, sometimes being mistaken for a simple need for new glasses. However, recognizing the early signs is crucial for timely diagnosis and management, which can help preserve vision long-term.
Blurry or Distorted Vision
The most common early symptom is a gradual blurring of vision that cannot be fully corrected. You might notice that straight lines, like door frames or power lines, appear wavy or bent. Words on a page or screen may seem to run together or have a slight shadow. This distortion occurs because the irregular corneal surface scatters light instead of focusing it cleanly. Initially, this may only affect one eye, but keratoconus typically impacts both eyes, though often to different degrees.
Frequent Changes in Glasses Prescription
If you find yourself needing a stronger prescription for your glasses or contact lenses every year, it could be a sign of an underlying issue. In a stable eye, prescriptions tend to remain relatively consistent for several years, especially after your early twenties. With keratoconus, the cornea is continually changing shape, causing your level of short-sightedness and astigmatism to increase. This progression means that a prescription that worked well a few months ago may no longer provide clear vision. Rapid and frequent prescription changes are a key indicator that warrants a more thorough corneal evaluation.
Light Sensitivity and Glare
Increased sensitivity to light, also known as photophobia, is another common symptom. Bright sunlight or overhead fluorescent lights can feel overwhelming and cause discomfort or headaches. This occurs because the irregular corneal surface scatters light more broadly inside the eye, rather than focusing it neatly. At night, this scattering effect creates significant glare, halos, or starbursts around headlights and streetlights, making driving difficult and uncomfortable.
Difficulty Seeing Clearly at Night
Night vision problems are often one of the first things people with early keratoconus notice. The combination of low light and bright light sources (like headlights) exaggerates the visual distortions caused by the cone-shaped cornea. The glare and halos around lights can be distracting and may reduce your ability to see other objects on the road or in your surroundings. This can make night driving feel unsafe long before daytime vision is significantly impacted.
What Vision Looks Like With Keratoconus
As keratoconus progresses, the visual disturbances become more pronounced. What begins as mild blurriness can evolve into distinct and disorienting distortions that interfere with daily activities like reading, driving, and recognizing faces.
Ghosting or Double Images
One of the hallmark symptoms of keratoconus is monocular diplopia, which means seeing double or multiple images with just one eye. This is often described as "ghosting," where you see a faint, overlapping copy of an object trailing its edge. For example, when looking at a stop sign, you might see the primary red sign with a faint, shadowy replica slightly offset from it. This effect is caused by the irregular cornea splitting a single light beam into multiple paths, creating several images on the retina instead of one sharp image.
Halos and Starbursts Around Lights
The scattering of light by the irregular corneal surface is most noticeable at night. A single point of light, like a streetlight, may appear as a large, blurry halo or a starburst with streaks of light radiating outwards. These visual artifacts are not just distracting; they can significantly impair vision in low-light conditions. Driving at night becomes particularly challenging because the glare from oncoming headlights can obscure the road ahead, making it difficult to judge distances and see other vehicles or pedestrians.
Why Standard Glasses May Stop Working
Standard glasses and conventional soft contact lenses are manufactured to correct for uniform refractive errors on a smooth, regularly shaped cornea. They work by bending light in a predictable way to compensate for myopia, hyperopia, or regular astigmatism.
In keratoconus, the cornea is irregularly shaped. The steepness and curvature can vary dramatically across different parts of the cornea. A standard spectacle lens cannot correct for this complex, localized distortion. While glasses may help in the very early stages, they quickly become ineffective as the cornea becomes more cone-shaped. You may find that even with a brand-new prescription, your vision remains blurry and distorted because the lenses cannot account for the underlying corneal irregularity. This is when specialized contact lenses become necessary.
What Causes Keratoconus?
The exact cause of keratoconus is not fully understood, but it is believed to result from a combination of genetic and environmental factors. Research suggests that these elements work together to weaken the corneal structure, leading to the characteristic thinning and bulging.
Genetic Factors
Genetics play a significant role. About 1 in 10 people with keratoconus has a parent who also has the condition. This indicates a hereditary link, where certain genes may predispose an individual to weaker corneal tissue. If you have a family history of keratoconus, it is important to have regular eye examinations that include corneal imaging, even if you do not have symptoms. Early detection allows for prompt management that can help stabilize the cornea before significant vision loss occurs.
Eye Rubbing and Environmental Triggers
Chronic and vigorous eye rubbing is strongly associated with the development and progression of keratoconus. The physical pressure of rubbing can stress and weaken the corneal tissue over time, especially in individuals who are already genetically predisposed. People with allergies, hay fever, or eczema are more prone to itchy eyes and, therefore, more likely to rub them. Managing these underlying allergic conditions with antihistamine eye drops or other treatments can help reduce the urge to rub and lower the risk of damaging the cornea.
Why Keratoconus Often Appears in the Teenage Years
Keratoconus typically manifests during puberty and progresses through the teenage years and into the early thirties. This timing suggests that hormonal changes during adolescence may play a role in triggering the condition in susceptible individuals. The combination of genetic predisposition and hormonal shifts may activate the processes that lead to corneal thinning. Once it begins, the condition can progress for 10 to 20 years before stabilizing in most people.
Can Keratoconus Be Detected Early?
Yes, absolutely. With modern diagnostic technology, keratoconus can be detected in its earliest stages, often before you notice any significant symptoms. Early detection is the key to effective management, as it allows for interventions that can slow or halt the progression of the condition.
How Advanced Corneal Imaging Helps Diagnose Keratoconus
The most important tool for diagnosing keratoconus is corneal topography, also known as corneal mapping. This advanced imaging technology creates a detailed, three-dimensional map of the surface of your cornea. At NVISION Eyecare, we use sophisticated instruments like the EIDON wide-field retinal camera and Optical Coherence Tomography (OCT) to get a precise picture of your eye health.
A corneal topographer measures thousands of points across the cornea to map its shape and curvature. The resulting map uses a color-coded scale to show variations in steepness. A normal cornea will show a relatively uniform, rounded pattern. In early keratoconus, the map will reveal a localized area of steepening, typically in the lower portion of the cornea, which is the first sign of the cone developing. This technology can detect subtle changes that would be invisible during a standard eye exam.
Why Early Diagnosis Matters
Diagnosing keratoconus early is critical for several reasons:
- Preserving Vision: The primary goal of early treatment is to stop the cornea from becoming more distorted. Interventions like corneal cross-linking are most effective when performed before significant thinning and scarring have occurred.
- Slowing Progression: Catching the condition early allows us to monitor its progression closely and intervene at the right time. This proactive approach can prevent the need for more invasive procedures later on.
- Better Vision Correction: In the early stages, vision can often be corrected with specialty soft or rigid gas permeable lenses. If the condition progresses, more complex and customized lenses, such as scleral lenses, may be required.
- Avoiding Complications: Advanced, untreated keratoconus can lead to corneal scarring or a condition called hydrops, where a break in the cornea causes sudden, painful vision loss. Early management helps prevent these complications.
How Keratoconus Is Diagnosed During an Eye Exam
A comprehensive eye examination is the first step in diagnosing keratoconus. While a standard vision test might raise suspicion due to frequent prescription changes, specialized tests are needed for a definitive diagnosis.
Corneal Topography and Mapping
Corneal topography is the gold standard for diagnosing keratoconus. During this non-invasive test, you will rest your chin on a machine and look at a lighted target. The device projects a series of illuminated rings onto your cornea, and a camera captures the reflection. A computer then analyzes the pattern of the reflected rings to generate a detailed topographical map. This map clearly shows the shape, curvature, and thickness of your cornea, allowing your optometrist to identify any tell-tale signs of conical bulging, even at the sub-clinical stage.
Other Tests Your Optometrist May Use
In addition to corneal topography, your optometrist may perform other tests to assess your corneal health and vision:
- Slit-Lamp Examination: Using a high-magnification microscope called a slit lamp, your optometrist will examine your cornea for signs of keratoconus, such as thinning, scarring, or iron deposits at the base of the cone (known as a Fleischer ring).
- Pachymetry: This test measures the thickness of your cornea. In keratoconus, the cornea is thinner than normal, particularly at the steepest point of the cone. OCT technology can provide highly precise pachymetry maps.
- Refraction: A detailed refraction test will be performed to determine the best possible vision correction. The presence of high or irregular astigmatism that cannot be fully corrected with glasses is a strong indicator of keratoconus.
Treatment Options for Keratoconus
The goal of keratoconus treatment is two-fold: first, to provide clear and comfortable vision, and second, to slow or stop the progression of the condition. Treatment options vary depending on the severity and progression of the keratoconus.
Specialty Contact Lenses
For most people with keratoconus, specialty contact lenses are the primary method of vision correction. Unlike standard soft lenses, these lenses are designed to vault over the irregular corneal surface and create a new, smooth refractive surface.
- Rigid Gas Permeable (RGP) Lenses: These are small-diameter hard lenses that rest on the cornea. They are made of a durable, oxygen-permeable material that holds its shape, effectively masking the corneal irregularity. The space between the RGP lens and the cornea fills with tears, creating a smooth optical surface that corrects vision.
- Hybrid Lenses: These lenses offer the best of both worlds: a rigid gas permeable center for crisp optics and a soft outer skirt for comfort similar to a standard soft lens. They can be a great option for those who find RGP lenses uncomfortable.
Scleral Lenses for Advanced Keratoconus
For moderate to advanced keratoconus, or for those who cannot tolerate smaller lenses, scleral lenses are often the ideal solution. These are large-diameter gas permeable lenses that vault completely over the entire cornea and rest on the sclera (the white part of the eye).
Because they do not touch the sensitive corneal tissue, scleral lenses are exceptionally comfortable. The space between the back of the lens and the cornea is filled with a sterile saline solution, which not only corrects the irregular optics but also provides constant hydration to the eye. This makes them an excellent choice for patients who also suffer from dry eye. Scleral lenses can provide outstanding vision even in cases of severe corneal irregularity.
Corneal Cross-Linking
Corneal cross-linking (CXL) is a revolutionary procedure designed to halt the progression of keratoconus. It is not a vision correction procedure but a therapeutic treatment to strengthen the cornea. The procedure involves applying riboflavin (vitamin B2) eye drops to the cornea and then activating them with a controlled dose of ultraviolet (UV) light. This process creates new collagen cross-links within the cornea, making it stiffer and more resistant to further bulging. CXL is most effective in younger patients whose keratoconus is still progressing and can prevent the need for more invasive surgery in the future.
When Surgical Options May Be Considered
In a small percentage of cases where keratoconus is very advanced, has led to significant scarring, or cannot be managed with contact lenses, surgical options may be explored.
- Corneal Ring Segments (Intacs): These are small, transparent plastic arcs that are surgically inserted into the mid-layer of the cornea. They work by flattening the central cornea, reducing the cone's steepness and improving vision.
- Corneal Transplant (Keratoplasty): In the most severe cases, a corneal transplant may be necessary. This involves replacing the damaged cornea with healthy donor tissue. This is typically considered a last resort when all other treatment options have failed.
When to See an Optometrist About Keratoconus
Regular eye exams are essential for everyone, but certain signs should prompt you to schedule an appointment specifically to check for keratoconus.
Signs You Should Schedule an Eye Exam
You should book an eye exam if you experience any of the following:
- Vision that is becoming progressively blurrier or more distorted.
- Frequent changes in your glasses or contact lens prescription.
- New or worsening glare, halos, or sensitivity to light.
- Seeing double or ghost images out of one eye.
- A family history of keratoconus.
- Difficulty achieving clear vision even with new glasses.
If you are experiencing any of these symptoms, a comprehensive eye examination with corneal topography is the best way to determine the cause and get the right care.
Keratoconus Care and Management in Auckland
At NVISION Eyecare in Auckland, we specialize in the diagnosis and non-surgical management of keratoconus. Our clinic is equipped with advanced diagnostic technology, including corneal topography and OCT, to detect keratoconus at its earliest stage. Dr. Ryan Mahmoud has extensive experience in fitting specialty contact lenses, including custom RGP, hybrid, and scleral lenses.
Our approach is centered on personalized care. We take the time to map your cornea precisely and conduct a detailed fitting process to find the lens that provides the best possible vision and comfort for your unique eyes. We work closely with our patients to monitor their corneal health and manage their condition effectively for the long term. If you are concerned about keratoconus, we are here to provide expert guidance and state-of-the-art care.
Frequently Asked Questions About Keratoconus
Is keratoconus hereditary?
Yes, there is a genetic component to keratoconus. Approximately 10% of individuals with the condition have a family member who is also affected. If keratoconus runs in your family, it is recommended that you and your close relatives undergo regular screenings, including corneal topography, to check for early signs of the condition.
Does keratoconus always get worse?
Keratoconus is a progressive condition, meaning it does tend to worsen over time, especially during the teenage years and early twenties. However, the rate of progression varies significantly from person to person. For many, the condition naturally stabilizes in their 30s or 40s. Treatments like corneal cross-linking are specifically designed to halt this progression and are highly effective.
Can keratoconus cause blindness?
Keratoconus does not cause total blindness in the sense of seeing complete darkness. However, if left untreated, it can lead to severe vision impairment that cannot be corrected with glasses, making it difficult to perform daily tasks like reading or driving. In very advanced cases, it can cause legal blindness. With modern treatments, severe vision loss from keratoconus is largely preventable.
Can people with keratoconus wear contact lenses?
Yes, specialty contact lenses are the primary and most effective way to correct vision for people with keratoconus. Standard soft contact lenses usually do not work well because they simply drape over the irregular cornea. However, custom-designed lenses such as rigid gas permeable (RGP) lenses, hybrid lenses, and scleral lenses are specifically made to vault over the irregular corneal shape, creating a smooth optical surface and providing clear, crisp vision.